 The proximal port,
commonly termed the CVP port, is used to measure
right atrial or central venous pressure. It is also used for medication infusion
and fluid boluses for cardiac output measurement.
The proximal port,
commonly termed the CVP port, is used to measure
right atrial or central venous pressure. It is also used for medication infusion
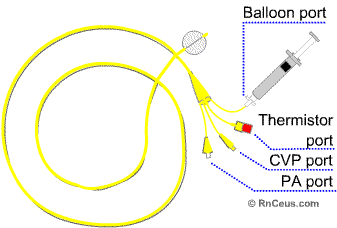
and fluid boluses for cardiac output measurement.Components of the Pulmonary Artery Catheter
 The proximal port,
commonly termed the CVP port, is used to measure
right atrial or central venous pressure. It is also used for medication infusion
and fluid boluses for cardiac output measurement.
The proximal port,
commonly termed the CVP port, is used to measure
right atrial or central venous pressure. It is also used for medication infusion
and fluid boluses for cardiac output measurement.
The distal port is used for PA pressure measurements and PCWP measurements when the balloon is inflated. Mixed venous blood gases can also be drawn from this port. The balloon port which is located at the tip of the catheter is inflated with a small amount of air (less than 1.5cc). When inflated, this balloon allows the catheter to float into a pulmonary artery branch vessel. This is refered to as a wedge position. This position allows pressure measurements to be made that indirectly reflect left ventricular end diastolic pressure.
The thermistor port is connected to the patient’s monitor via a cable and allows the display of continuous temperature readings. These temperature readings are essential to calculate cardiac output measurements. The actual thermistor is located just proximal to the balloon. In order to determine the cardiac output value, cool injectate is delivered rapidly through the proximal port of the PA catheter. A temperature curve is plotted over time as the cool injectate causes the pulmonary artery temperature to fall. It then rises back to the previous core temperature as warm blood continues in circulation.
Click here to open a new page and visit
the London Health Sciences Critical Care website for a detailed cardiac output
procedure and rationale.
(When your finished, close the page to return to your place at RnCeus.com)
Reduce Catheter Related Bloodstream Infections (CR-BSI) |
|
The PA catheter is inserted by a physician with the assistance of the critical care RN. Patient safety requires strict adherence to your facility policy and procedure when assisting line insertion.
While the PA catheter is inserted, the monitor will display
the various pressure waveforms associated with the catheter’s position
in the heart and vessels. The following section will discuss hemodynamic waveforms
and their interpretation.
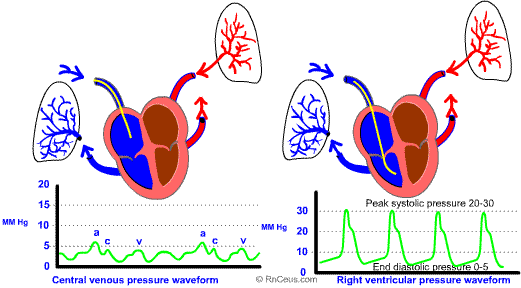
During the insertion procedure, the first waveform will be the right atrial
pressure. This wave will resemble a CVP wave. The following waveform
will be the right ventricular pressure as the catheter passes through
the right ventricle. During this time, the patient may experience some ventricular
dysrhythmias that disappear as soon as the catheter exits the right ventricle.
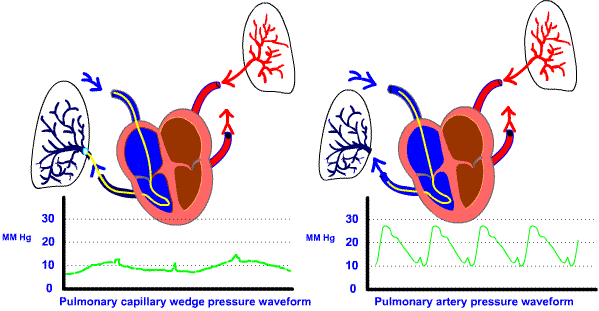
The catheter will enter the pulmonary artery and this will be its resting
place for the majority of the time. Finally, when the balloon is inflated, the
catheter will float into the pulmonary capillary and the resulting waveform
will be the wedge pressure. The following diagrams illustrates the waveforms
associated with inserting the pulmonary artery catheter.