Initial
Bladder Management after SCI
The immediate and early effects
of SCI on bladder function are quite different from those that follow recovery
from the initial injury. During the initial phase of spinal cord injury, the patient
is experiencing "spinal shock." Basically, spinal shock is the result
of swelling of the spinal cord. This swelling causes the inhibition of all reflexes
below the level of the injury, making the bladder "atonic" or "flaccid."
All reflexes are depressed, and the bladder cannot contract and empty.
For this reason, the best
plan for bladder management at this stage is use of a urinary catheter. During
this time, in response to IV fluids and posttraumatic changes in fluid balance,
there are generally large fluctuations in urine output.
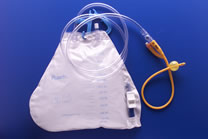 Catheterization
is achieved by insertion of a small-diameter latex or silicone tube into the
bladder through the urethra. It prevents overdistention of the bladder, and
consequently prevents injury to urinary structures. During initial stages, the
catheter is either left "indwelling" (a "retention"
or "foley" catheter) or is inserted intermittently ("ICs")
with aseptic technique. Other methods of management may be adopted based on
results of further patient assessment, such as frequency of UTIs and client
compliance
Catheterization
is achieved by insertion of a small-diameter latex or silicone tube into the
bladder through the urethra. It prevents overdistention of the bladder, and
consequently prevents injury to urinary structures. During initial stages, the
catheter is either left "indwelling" (a "retention"
or "foley" catheter) or is inserted intermittently ("ICs")
with aseptic technique. Other methods of management may be adopted based on
results of further patient assessment, such as frequency of UTIs and client
compliance
Instant
Feedback:
Bladder
management for a patient in spinal shock is frequently urinary catheterization.
Spinal shock, or depression
of the reflexes, generally lasts from 1 to 2 months, when the spinal reflexes
return. Reflexes may even become hyperactive.
Suggested guidelines, and
practical tips, for initial bladder management after SCI include:
- With acute overdistention
of the bladder, no more than 1000 cc of urine should be removed from the bladder
at one time. The theory behind this is that removal of more than 1000 cc suddenly
releases pressure on the pelvic blood vessels. This can affect overall circulatory
function and acute blood pressure changes can follow.
- Once the patient is no
longer receiving IV fluid (fluid output no more than about 100 cc/hour and
no problems with orthostatic hypotension), intermittent catheterization can
begin. ICs usually are started on a schedule of every 4 hrs. The schedule
for ICs is based on the patient's urine volumes. In most protocols, ICs are
maintained every 4 hours until that patient has gone 48 hours without a volume
over 500 ccs. At that point, the schedule of ICs goes to every 6 hours. The
patient should be reminded that it is important for the bladder to maintain
volumes under 500 ccs.
- Intermittent catheterization,
when properly used, prevents bladder overdistention and urethral irritation.
It also allows the patient more freedom of activity. By allowing the bladder
to fill, it also prevents bladder muscle atony. When a patient is in spinal
shock, this procedure should be done aseptically.
- If the
SCI injury is above T12, the patient may learn to "reflex" void.
In this case, the bladder may try to empty by reflex, or "bearing down",
without input from the brain. It may take 2 to 3 months after the initial
injury for this to begin to occur. If the patient is voiding by "reflexing",
the patient may decrease the number of ICs.
Instant
Feedback:
It's
important that the amount of urine in the bladder not exceed about 300 cc.
© RnCeus.com
 Catheterization
is achieved by insertion of a small-diameter latex or silicone tube into the
bladder through the urethra. It prevents overdistention of the bladder, and
consequently prevents injury to urinary structures. During initial stages, the
catheter is either left "indwelling" (a "retention"
or "foley" catheter) or is inserted intermittently ("ICs")
with aseptic technique. Other methods of management may be adopted based on
results of further patient assessment, such as frequency of UTIs and client
compliance
Catheterization
is achieved by insertion of a small-diameter latex or silicone tube into the
bladder through the urethra. It prevents overdistention of the bladder, and
consequently prevents injury to urinary structures. During initial stages, the
catheter is either left "indwelling" (a "retention"
or "foley" catheter) or is inserted intermittently ("ICs")
with aseptic technique. Other methods of management may be adopted based on
results of further patient assessment, such as frequency of UTIs and client
compliance