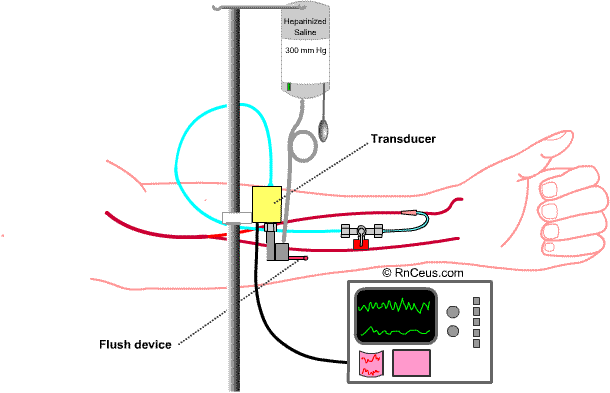
Arterial Blood Pressure Monitoring
A secondary benefit of an art line is the ability to do serial blood sampling. Arterial blood gas evaluations can be performed without the need for repeated painful needle sticks. Arterial blood gas monitoring is vital to the successful treatment of respiratory failure, whatever the cause.
Arterial pressure monitoring begins with an accurate patient history and assessment. A history of peripheral vascular disease could raise the risk of complications from arterial line insertion. Skin changes, scars, sores, discoloration, swelling, excess warmth or swelling etc., could indicate the presence of peripheral vascular disease.
Palpation, capillary refill and the Allen test are necessary steps to determine the suitability of a limb for insertion of an arterial line. The Allen test determines the patency of the arm's radial and ulnar arteries. The Allen test must be done prior to arterial line insertion, in order to reduce the risk of ischemia due to arterial occlusion.
Follow your institutional guidelines when inserting or assisting in the placement of an arterial line. The necessary equipment for placement will include:
Once the catheter is inserted, it is connected to the flushed and airless tubing/transducer assembly. The transducer should be positioned level with the heart, then zeroed to negate the pressure applied by the heparinized flush. When zeroed, the transducer will reflect changes in the intra-arterial pressure.

Waveform evaluation is the best method to determine correct placement.
A normal wave form will be:
Correlation of pressure readings with blood pressure cuff should be done periodically, if possible.
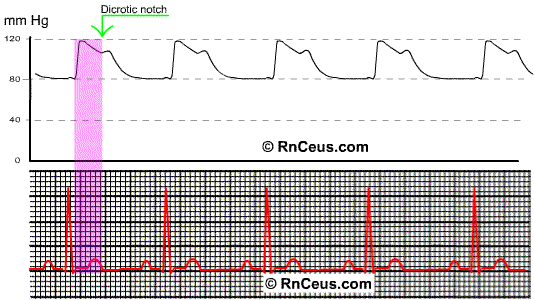
The normal peripheral arterial waveform will display the peak systolic pressure after the QRS. This phenomenon reflects the time it takes the cardiac systolic pressure wave to reach the peripheral catheter and sensor. The dicrotic notch reflects the closure of the aortic valve. Of course, the same time delay applies to the dicrotic notch. The aortic valve has closed prior to the display of the notch.
The time delay is a function of both distance and compliance or elasticity of the vessels. The waveform of a patient with arteriosclerotic disease would be steeper in ascent and descent, therefore shorter in duration and the notch would be less well defined.
Instant
Feedback