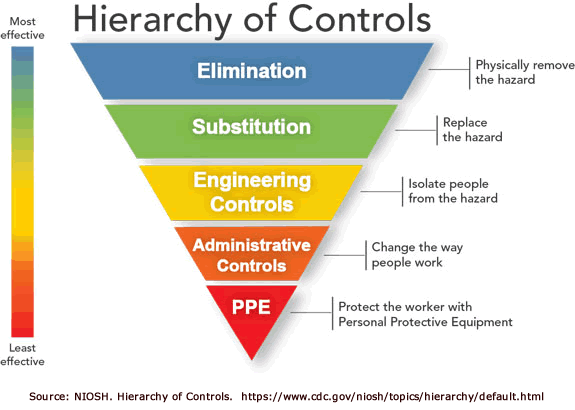
 NIOSH recommends minimizing exposure to HD's through primary prevention measures such as engineering controls, administrative controls, and personal protective equipment (PPE).
NIOSH recommends minimizing exposure to HD's through primary prevention measures such as engineering controls, administrative controls, and personal protective equipment (PPE)."Health care workers who prepare or administer hazardous drugs (e.g., those used for cancer therapy, and some antiviral drugs, hormone agents, and bioengineered drugs) or who work in areas where these drugs are used may be exposed to these agents in the workplace. About 8 million U.S. healthcare workers are potentially exposed to hazardous drugs, including pharmacy and nursing personnel, physicians, operating room personnel, environmental services workers, workers in research laboratories, veterinary care workers, and shipping and receiving personnel (CDC 2020)."
"Many hazardous drugs used to treat cancer (for example, alkylating agents) bind to or damage DNA. Other antineoplastic drugs, some antivirals, antibiotics, and bioengineered drugs interfere with cell growth or proliferation, or with DNA synthesis. In some cases, the nonselective actions of these drugs disrupt the growth and function of both healthy and diseased cells, resulting in toxic side effects for treated patients and their offspring. These nonselective actions can also cause adverse effects in health care workers who are inadvertently exposed to hazardous drugs (NIOSH 2016)." The National Institute for Occupational Safety and Health hazardous considers a drug to be hazardous if it exhibits one or more of the following six characteristics in humans or animals:
Workplace exposures to hazardous drugs (HDs) can cause both acute and chronic health effects including: skin rashes, adverse reproductive outcomes (including infertility, spontaneous abortions, and congenital malformations), and possibly leukemia and other cancers. Health risks depend on how much exposure a worker has to these drugs and how toxic they are. NIOSH recommends implementation of a practice-specific Standard Precautions approach to handling hazardous drugs safely (NIOSH 2016).
PREVENTING HEALTH CARE WORKERS EXPOSURE TO HAZARDOUS DRUGS.
 NIOSH recommends minimizing exposure to HD's through primary prevention measures such as engineering controls, administrative controls, and personal protective equipment (PPE).
NIOSH recommends minimizing exposure to HD's through primary prevention measures such as engineering controls, administrative controls, and personal protective equipment (PPE).
- Engineering controls include: biological safety cabinets (BSC), compounding aseptic containment isolators, closed system transfer devices, and needleless systems.
- Administrative controls include implementing work practices, management policies, and training programs to reduce worker risk. A medical monitoring program serves as a form of secondary prevention by identifying indicators of exposure or early disease.
- PPE should be used when engineering controls and/or administrative controls are not feasible in reducing exposures to hazardous drugs or when other control measures are not available or practical. PPE should always be used in the context of an overall health and safety program that provides adequate training, retraining, and periodic testing of the workers’ knowledge of the proper use of PPE.
- Gowns should not have seams or closures that could allow drugs to pass through. They should have long sleeves with tight fitting cuffs. Disposable gowns made of polyethylene-coated polypropylene or other laminate materials offer better protection than those of non-coated materials. Cloth laboratory coats, surgical scrubs, or other absorbent materials permit the penetration of hazardous drugs, and can hold spilled drugs against the skin and increase exposure.
- Dispose of gowns after each use. Reusing gowns increases the likelihood of exposure to hazardous drugs.
- Wear gowns whenever there is a possibility of splash or spill as in compounding or administration of hazardous drugs.
- Do not wear gowns outside the compounding or administration area to avoid spreading drug contamination to other areas and possibly exposing non-protected workers.
- If no permeation information is available for the gowns you use, change them every 2 to 3 hours or immediately after a spill or splash.
- Gloves - "it is important to rely on test information provided by the glove manufacturer that demonstrates permeation resistance to specific hazardous drugs." "polyvinyl chloride exam gloves offer little protection against drug exposures".
- Inspect gloves for defects before use and change gloves on a regular basis. Changing recommendations vary from 30-60 minutes. Whenever gloves are damaged or contact with a drug is known or suspected, carefully remove and dispose of them properly.
- Use powder-free gloves since the powder can contaminate the work area and can adsorb and retain hazard- ous drugs.
- Wear two pairs of gloves when compounding, administering, and disposing of hazardous drugs.
- Sterile chemotherapy gloves are required for compounding of sterile preparations under USP Chapter <797>.
- Wear the inner glove under the gown cuff and the outer glove over the cuff. Place gloves with long cuffs over the cuff of the gown to protect the wrist and forearm.
- When compounding sterile preparations; sanitize gloves with sterile 70% alcohol spray or gel and allow them to dry; ensure that the selected gloves are not degraded by alcohol.
- When removing double gloves, turn gloves inside-out so that contaminated surfaces do not touch uncontaminated surfaces.
- Wash hands thoroughly with soap and water both before donning and after removing gloves.
- Eye and Face Protection - Proper eye and face protection is needed whenever hazardous drugs may splash in the eyes since many hazardous drugs are irritating to eyes and mucous membranes and may be absorbed by the eyes.
- Use eye and face protection when compounding a drug outside the BSC or isolator (e.g., in the operating room), working at or above eye level, cleaning a BSC or containment isolator, or cleaning a spill.
- Use face shields in combination with goggles to provide a full range of protection against splashes to the face and eyes. Face shields alone do not provide full eye and face protection.
- Do not use eye glasses or safety glasses with side shields, as they do not offer adequate protection to the eyes from splashes.
- A full-facepiece respirator also provides eye and face protection
- Respiratory Protection - For most activities requiring respiratory protection, a NIOSH-certified N-95 or more protective respirator is sufficient to protect against airborne particles; however, these respirators offer no protection against gases and vapors and little protection against direct liquid splashes. A surgical N-95 respirator provides the respiratory protection of an N-95 respirator and the splash protection provided by a surgical mask. Surgical masks alone do not provide respiratory protection from drug exposure and should not be used to compound or administer drugs.
- Use an appropriate full-face piece chemical cartridge-type respirator for events such as large spills when an intravenous (IV) bag breaks or a line disconnects and leaks, or where there is known or suspected airborne exposure to vapors or gases
Spills
Emergency procedures to cover spills or inadvertent release of hazardous drugs should be included in the facility's overall health and safety program. A properly protected person trained in the appropriate procedures should clean up spills and breakages immediately. The area should be identified with a warning sign to limit access to the area. An incident reports should be filed to document the spill and persons exposed.
PPEs should be worn by all staff handling patient excreta (urine, vomit, feces) for seven days after the administration of chemotherapy:
- plastic apron
- gloves (U.S. Dept. of Labor n.d.)
References
Boiano, J. M., Steege, A. L., & Sweeney, M. H. (2014). Adherence to safe handling guidelines by health care workers who administer antineoplastic drugs. Journal of occupational and environmental hygiene, 11(11), 728–740. https://doi.org/10.1080/15459624.2014.916809
Centers for Disease Control and Prevention (2020). Hazardous drug exposures in health care. Centers for Disease Control and Prevention. [ last reviewed: May 4, 2020] Retrieved January 13, 2022, from https://www.cdc.gov/niosh/topics/hazdrug/
NIOSH (2016). NIOSH list of antineoplastic and other hazardous drugs in healthcare settings, 2016. By Connor TH, MacKenzie BA, DeBord DG, Trout DB, O’Callaghan JP. Cincinnati, OH: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, DHHS (NIOSH) Publication Number 2016-161 (Supersedes 2014-138)
NIOSH - WORKPLACE SOLUTIONS (2009) Personal Protective Equipment for Health Care Workers Who Work with Hazardous Drugs. Accessed online 1/17/2022. http://www.cdc.gov/niosh/docs/wp-solutions/2009-106/pdfs/2009-106.pdf
United States Department of Labor. Hazardous Drugs - Controlling Occupational Exposure to Hazardous Drugs | Occupational Safety and Health Administration. (n.d.). Retrieved January 17, 2022, from https://www.osha.gov/hazardous-drugs/controlling-occex#spills
© RnCeus.com