The Physiology of High Altitude
Hypoxia is the primary factor involved in the development of high altitude illness. Acute hypoxia strongly stimulates the sympathetic system and depresses the parasympathetic. The autonomic nervous system senses and responds to acute hypoxia by increasing ventilation, heart rate, cardiac output and catecholamine levels.
The ability to progressively increase ventilation and cardiac output throughout ascent is a characteristic of travelers who are less likely to experience high altitude illness. Each traveler has a unique capacity to intensify response to hypoxia. The rate of ascent and individual adaptive profile will largely determine response to acute hypobaric hypoxia.
Lowland Breathing
Automatic and rhythmic discharges generated within the respiratory centers of the medulla oblongata and pons are responsible for normal involuntary ventilatory muscle contractions. Inspiratory neurons transmit these discharges to contract the diaphragm via the phrenic nerves and intercostal muscles via the intercostal nerves. Expiratory nerves inhibit inspiratory discharge allowing air to be passively expelled as the muscles relax. Impulses from stretch receptors in the lungs, via the vagus nerve, also inhibit inspiration.
At sea level where oxygen is plentiful, central chemoreceptors located in the medulla predominate. Central chemoreceptors are responsible for the majority of the hypoxic ventilatory response (HVR). These receptors respond to decreased CSF pH by increasing the rate and depth of inspiration. The pH of CSF falls when the CO2 level of plasma increases. At sea level these receptors maintain resting PaCO2 around 40mmHg. When PaCO2 rises, ventilation increases pH and PaO2 by driving off the excess CO2. Kidneys increase output to eliminate excess HCO3 lowering pH towards normal.
![]()
Hypobaric Hypoxic Breathing
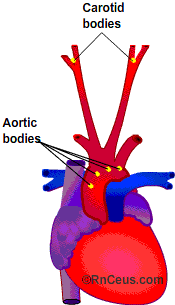 At high altitude the body struggles to meet O2 requirements. The lowland breathing strategy employing central pH receptors can get the traveler only so far. As ventilation increases, PaCO2 drops, pH increases and the central receptor activity subsides.
At high altitude the body struggles to meet O2 requirements. The lowland breathing strategy employing central pH receptors can get the traveler only so far. As ventilation increases, PaCO2 drops, pH increases and the central receptor activity subsides.
Peripheral chemoreceptors located in the carotid and aorta take over when central receptor stimulation lags. These peripheral receptors provide additional HVR and respond to ![]() CO2,
CO2, ![]() H+ ions and
H+ ions and ![]() O2 in plasma. When plasma H+ ions
O2 in plasma. When plasma H+ ions ![]() or O2
or O2![]() below PaO2 of 60 mmHg they are able to boost HVR.
below PaO2 of 60 mmHg they are able to boost HVR.
Nocturnal Cheyne-Stokes breathing is a common experience when sleeping at high altitude. It results from the fluctuations of PaO2 and PaCO2 that are exaggerated during sleep. The fluctuations cause alternating periods of apnea and hyperventilation.
Hemodynamic response to Acute Hypoxia
The body initiates compensatory strategies to improve tissue oxygenation in response to acute hypobaric hypoxia. Two of these strategies are hemoconcentration and increased cardiac output.
Hemoconcentration increases hemoglobin per unit of blood. This results in greater O2 carrying capacity. Hypoxia related hemoconcentration occurs through three main mechanisms, hypoxic diuretic response (HDR), hypoxia induced erythropoiesis and insensible water loss from hyperventilation.
Hypoxic diuretic response (HDR) begins to increase hematocrit within hours of hypoxic exposure. HDR inhibits renal tubular sodium reabsorption. It is currently believed to be related to an unknown hypoxia induced humoral factor, perhaps endothelin-1 or epinephrine.
Hypoxia induced erythropoiesis results from the release of renal erythropoietin (EPO). Epo stimulates the production of new RBC. There is a lag time of 2-3 days before the new cells begin to increase the hematocrit.
Water vapor loss during hyperventilation reduces plasma and increases hematocrit. Humidity at high altitude is usually very low and expired air contains about 6% water vapor.
Cardiac output increases in response to acute hypobaric hypoxia. Cardiac output equals heart rate multiplied by stroke volume (CO = HR X SV). It is believed that hemoconcentration elevates catecholamine levels causing increased heart rate. Given adequate time, the heart rate can increase enough to overcome the reduced stroke volume that results from increased vascular resistance caused by hemoconcentration and pulmonary arteriole constriction.
The pulmonary arterioles constrict in response to hypoxia. Pulmonary arteriole vasoconstriction may be an adaptation intended to protect lung vessels from the elevated pressure and flow that results when cardiac output is increased. But it can also be subject to maladaptation and appears to play an important role in the development of high altitude pulmonary edema (HAPE).
© RnCeus Interactive, LLC all rights reserved.